Feline osteoarthritis is one of the most common degenerative joint diseases in cats. In fact, 90% of cats over the age of 10 develop some kind of join disease. Scary numbers! If you have an older kitty – read up and learn more about feline osteoarthritis right now.
Background information
Feline osteoarthritis is a progressive type of a joint disease that causes pain and inflammation in cat’s synovial joints. The term osteoarthritis is often mixed up with “degenerative joint disease” or “DJD”. DJD is a broader term and includes all degenerative disorders affecting all types of joints. Osteoarthritis refers to the degenerative disorder of synovial joints only (Bennett, 2008).
So, what exactly is a synovial joint? A joint in general is a structure in the feline body where two bones are brought together and held in place by supporting tissues. Depending on the type of tissues that connect the bones, we recognize 3 types of joints: synovial, fibrous and cartilaginous. Synovial joints are with the greatest range of movement, such as knees, elbows and wrists.
In a synovial joint, the bone ends are covered with cartilage – firm and flexible connective tissue. Cartilage doesn’t have any nerves, so it ensures that there is no pain when the two bones touch each other. The area between the bone ends is enclosed by the joint capsule, and the cavity between them is filled with synovial fluid. The ligaments may be placed as the part of the joint capsule, as well as inside or outside of it and they help hold the bones in alignment (PetCoach, Petco Animal Supplies Stores, Inc., 2018a).
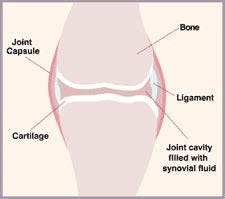
Figure 1: Synovial joint in cats (PetCoach, Petco Animal Supplies Stores, Inc., 2018a).
Osteoarthritis is ultimately caused by the loss of the cartilage at the ends of the bones in a synovial joint. Without the cartilage, the bone ends are now exposed and when they get in touch it results in pain and inflammation. Additionally, small bony projections called osteophytes appear on the bone close to the joint – causing even more pain.
Osteoarthritis in cats is usually associated with cat’s age and often affects cats over 10 years of age. This is what we call primary osteoarthritis. However, osteoarthritis may also occur as a result of other factors affecting the joint – for example previous trauma, infectious diseases or hip dysplasia. This is secondary osteoarthritis. Hip dysplasia accounts for about 22% of cases of feline osteoarthritis (PetCoach, Petco Animal Supplies Stores, Inc., 2018b) (Lappin, 2001).

Feline osteoarthritis is one a common joint disease in older cats
How common is osteoarthritis in cats?
The rate of degenerative joint diseases in general is significantly high among cats. For example, Hardie E.M. et al. examined radiographs of 100 geriatric cats looking for radiographic evidence of DJD in a study published in 2002. The study was conducted from 1994 to 1997 and included cats older than 12 years of age.
The results showed evidence of DJD in 90% of examined cats (Hardie, Roe, & Martin, 2002), and osteoarthritis is thought to be the most common of all feline degenerative joint diseases. In 2005, Clarke et al. examined 218 cats of all ages. They found a prevalence of 16.5% of appendicular osteoarthritis and a total prevalence of radiographic DJD including all categories of 33.9% (Bennett, 2008).
Which cats are more prone to osteoarthritis?
Although it can also occur in younger cats, this is a disease that most frequently affects senior felines.
How will I recognize if my cat is arthritic?
Even though the data states that many senior cats show radio-graphic evidence of the disease, its clinical signs are not yet well-documented. In general, arthritic cats may show overall stiffness, lameness, lethargy and decreased flexibility.
They may have trouble climbing or jumping and feel discomfort when posturing to urinate or defecate or when you pet or handle them in certain positions. You may notice changes in your cat’s behavior, such as decreased activity, reduced grooming, hesitancy to jump or run and changed litter box habits (Malik & Sparkes, 2010).

The main problem is that the behavioral changes associated with osteoarthritis can be easily missed due to the cat’s lifestyle. Our felines are often solitary animals who love to sleep a lot, and therefore inactivity due to the chronic joint pain is just very difficult to determine (Robertson, 2008).
How is feline osteoarthritis diagnosed?
Diagnosis of the feline osteoarthritis can be problematic. For instance, we have previously mentioned the study conducted by Hardie et al., where the researchers found radiographic evidence of DJD in 90% of all examined cats.
However, only 4 of these cats contained a mention of DJD in their medical records. Some cases of severe DJD were mistakenly diagnosed as neurological disorders (Robertson, 2008). These figures are terrifying as they show just how small the percentage of appropriately diagnosed arthritic cats really is!

When inspecting for osteoarthritis, veterinarians usually conduct a physical exam followed by examination of radiographs. Radiography is most commonly used in diagnosis of osteoarthritis because it provides a lot of valuable information.
Unfortunately, even on the x-ray, changes in the joint may be too subtle and hard to spot. This is why comparison of x-rays is highly recommended when conducting this method. Other tests that may be followed are complete blood count, chemistry panel, serologic tests, synovial fluid analysis and biopsy (PetCoach, Petco Animal Supplies Stores, Inc., 2018c).
Treatment of osteoarthritis
Once developed, osteoarthritis can’t be cured. But, there are ways we can make our arthritic cats more comfortable! Osteoarthritis treatment usually embraces steps to help relief the chronic joint pain, which can usually be treated in three different ways: through lifestyle changes and/or pharmacological and non-pharmacological interventions.
Lifestyle changes usually embrace controlled exercise, environmental modifications and weight loss for overweight cats. Pharmacological intervention refers to any prescribed drugs for treatment of the chronic joint pain.
NSAID and opioids are the most commonly used drug therapy for osteoarthritis. And lastly, nonpharmacologic intervention involve rehabilitation therapy (for example underwater treadmill), acupuncture and nutraceuticals (Robertson, 2008).
How can I make my kitty more comfortable?
Like any fur parent of an arthritic pet, you’re probably wondering if there’s anything you can do to help your beloved feline feel a little bit better. And fortunately, yes there is! You can make it easier for you kitty to reach its food, water and litter box by providing direct, easy and comfortable access. Maybe you can even treat it with a new, cozy and soft bedding.
Since arthritic cats find it difficult to groom themselves, help it by grooming the areas that are hard for it to reach. When your feline is calm and comfortable, try giving her a gentle massage to help relief the pain.

Feline osteoarthritis is a very common and painful condition among cats, and with awareness and knowledge, we may be able to provide them with longer and happier lives.
Citations:
Bennett, D. (2008). Feline osteoarthritis and degenerative joint disease (radiology). European Veterinary Conference Voorjaarsdagen, (pp. 179-180). Amsterdam, Netherlands.
Hardie, E., Roe, S., & Martin, F. (2002, March 1). Radiographic evidence of degenerative joint disease in geriatric cats: 100 cases (1994-1997).Journal of the American Veterinary Medical Association, 220(5), 628-32.
Lappin, M. (2001).Feline internal medicine secrets. Philadelphia: Hanley & Belfus.
Malik, R., & Sparkes, A. (2010). Synovial osteochondroma: an uncommon manifestation of a common disease. JFMS(12), 367-8.
PetCoach, Petco Animal Supplies Stores, Inc. (2018a). Normal Joint Anatomy in Cats. Retrieved March 14, 2018, from PetCoach
PetCoach, Petco Animal Supplies Stores, Inc. (2018b). Types of Arthritis in Cats. Retrieved March 14, 2018, from PetCoach
PetCoach, Petco Animal Supplies Stores, Inc. (2018c). Veterinary Procedures Used to Diagnose Joint Disease in Animals.
Retrieved March 14, 2018, from PetCoach
Robertson, S. (2008, November 1). Osteoarthritis in cats: What we now know about recognition and treatment. Retrieved March 14, 2018, from
